
Acute care physical therapy commonly gets overshadowed by more popular areas of interest such as outpatient orthopedics by students applying to physical therapy school. Many students and prospective students lack information or exposure to this area of practice which limits their interest. This is unfortunate because there are many benefits to acute care physical therapy that should be considered when choosing a career path. In this article we will go over many common questions, benefits, and drawbacks about working in acute care physical therapy with insight from Johns Hopkins employed physical therapists.
The opinions expressed from the therapists quoted in this article are of the individual therapists and DO NOT speak for, or represent the Johns Hopkins Hospital System as a whole.
*Disclaimer*
In my cohort of 70 physical therapy students at University of Maryland Baltimore’s DPT program only 2-3 students initially mentioned they had any interest in acute care physical therapy. This lack of interest in acute care physical therapy can be contributed to either lack of knowledge or understanding.
Many students applying and even currently in PT school, don’t know what acute care physical therapy is. I did 40 hours of shadowing in acute care, and even after 2 years of DPT curriculum I couldn’t picture what the work was like. It took until my first clinical internship my 3rd year in acute care to really grasp the concept of acute care physical therapy.
To start on a level playing field let’s start this article off with a basic understanding of acute care.
What is Acute care– In acute care, patients are seen that have a suffered an injury or illness that requires urgent and time sensitive medical care. This could be a broken bone, trauma (gunshot, stabbing, or car crash), or even a sudden health event such as a heart attack or stroke.
The goal of this level of care is to stabilize the patient enough to leave the hospital. This could accomplished in as little as a couple hours up to many months. Physical therapist’s play a crucial role in this setting.
What is the role of physical therapy in acute care?
As a physical therapist in acute care your job is to mobilize the patient as soon as they are medically stable and progress them to a level safe to leave the hospital. Early mobilization has been proven to decrease stay in the hospital as well as total healthcare utilization (1). This means you are getting patients home faster, saving them money, and decreasing the burden on the healthcare system as a whole.
You will be working as part of a team to help the patients regain their health and independence as quickly as possible. The medical doctors will diagnose the medical issues and stabilize the patient. The physical therapist has the unique role of improving health outcomes with movement and recommending very influential discharge recommendations for each patient.
Your training as a physical therapist gives you a unique point of view which you use to determine the best next step for the patient based on several contributing factors. You really challenge your clinical judgement by combining the patients diagnosis, prognosis, level of mobility, endurance, and the patients home factors such as family/friend support and home obligations.
Many times you have to make the recommendation that the patient is unsafe to go home after discharge from the hospital. Common recommendations other than home are subacute/acute rehabilitation centers, home with home-based physical therapy, home with outpatient therapy, or even nursing homes.
What is it like to work in acute care?
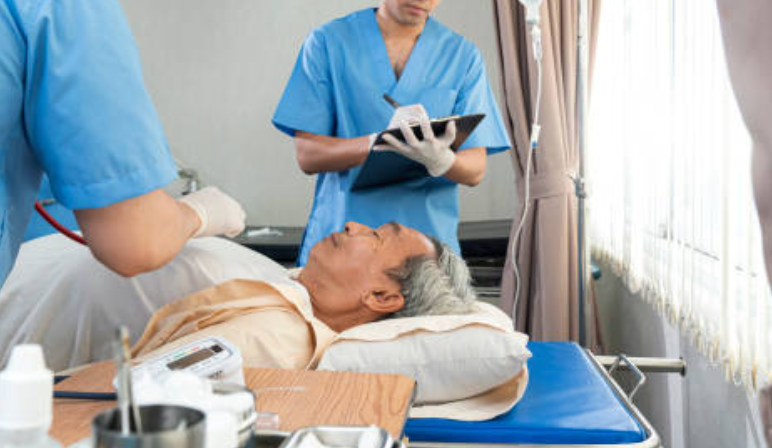
Acute care physical therapy is a very rewarding environment that is typically very flexible and provides a ton of variety that keeps therapists interested. In many hospitals therapists will be assigned a “floor”. Each floor hosts a specific category of patient that is being treated for different types of illnesses or injuries within that category. For example, patients with joint replacements will be found on the orthopedic floors and patients who survived a stroke will be found on the neurology floors.
According to the Johns Hopkins therapists that were surveyed for this post, they arrive to work between 7 and 10am and stay between 3 and 6pm. Their day usually begins with prioritizing which patients on your floor need to be seen and then reviewing their charts. The therapists will then decide if it is safe to see the patient and clarify safety precautions with the MD’s and RN’s.
What are the pro’s and con’s of acute care physical therapy.
Acute care physical therapy has its pro’s and con’s just like anything else in life. Here is what the therapists at Hopkins have to say about it.
Pro’s
- “I like the fast pace of work”
- “I love the feeling of being the first one to initiate mobility and gait training”
- “Inter-professional collaboration”
- “New learning everyday”
- “Flexibility”
- “Varied work experience”
Con’s/challenges
- “The schedule of the patient limiting the PT session”
- “Constant unknowns that impact productivity”
- “Medically unstable pt’s so you need to be more focused on red flags”
- “Schedule- 2 weekend days per month and holidays gets old!”
- “Not able to follow patients and see them progress”
So as you can see there are great things and not so great things about acute care. I think generally if you want new exciting things every week, flexibility over your schedule, and to see a reasonable amount of patients per day you will like acute care physical therapy.
On the other hand, if you want to see long term progress, avoid weekend and holiday work, and work with higher level patients you will want to settle into another area of practice.
Benefits of acute care physical therapy
As shown above acute care physical therapy has many benefits. It is great for those who like a fast paced work environment and want to collaborate with other professions. There is also a ton of flexibility and varied work experience.
Therapists from Johns Hopkins describe the work as “very rewarding” and say getting a patient from being “in a coma to ambulatory” is a great accomplishment.
Other benefits not mentioned above are the financial benefits of working in a hospital system. They can be more than other places such as private practice. For example, some therapist receive a pension and get tuition reimbursement for themselves and children. This is on top of standard benefits such as 401k matching, health insurance, and paid time off.
What is the difference between acute care and sub-acute physical therapy?
Acute physical therapy focus is on medical stabilization whereas sub-acute physical therapy the focus is on rehabilitation to a level safe enough to go home. In sub-acute physical therapy the rehab is more intense than the acute setting since the patient is now medically stable. The sessions average closer to 60 min vs shorter times in acute setting. They are also more specific to the physical limitations and goal of the patient. For example a goal could be increasing the amount of sit to stands performed in 30s to decrease the risk of falling in the home.
In the acute setting you will focus specifically functional tasks like rolling in bed, transferring from bed to chair, etc. This may sound simple, but it could take multiple session to get a patient from bed to chair with minimal support in this setting. In the acute setting other needs such as surgeries, imaging, and visits from MD’s supersede musculoskeletal conditioning.
What is the difference between inpatient and outpatient physical therapy?

In outpatient physical therapy the conditions seen are mostly sub-acute (several weeks to months old) or chronic (several months to years old). The focus of the training sessions are extremely specific and goals are typically is to improve function in the community or at home. You will not need to have as much focus on red flags and precautions as you would in the acute setting. At the same time you do not have immediate access to life saving medical teams so if their is a red flag you still need to be on your toes and catch it!
In the outpatient setting you will see the patient for a much longer time than the acute setting in most normal circumstances. Outpatient plan of cares can range from 4 weeks to 1 year depending on the diagnoses. Your clinic may also provide extra services that extend past the need of therapy and enter into preventative and maintenance care. This will be services much more closely related to personal training than physical therapy.
What are the productivity standards for acute care?
Productivity can vary from hospital to hospital, but in general you will be asked to see roughly 5-7 patients in an 8 hour day. By the very nature of this practice you will see patients one on one every session. This can be very appealing to someone working in other settings where you are expected to be double booked and see up to 20+ patients a day!
It is reasonable to expect productivity requirements of 2-3 units per patient you treat. This can be a challenge at times when working in the acute setting as you will treat patients who are at such a high medical complexity they can only tolerate 1 unit of treatment. This is where your skills come in to see how much more value you can offer to that patient to meet them where they are in their recovery.
This is in contrast to other clinics specifically “PT mills” which will not be named in this article. These clinics value profits over things such as quality care and their employee’s sanity. They expect 3 units from 15-20 patients a day not to count the time it takes to document for all of these patients. In the acute setting if you are efficient with your time you will have enough time to document and treat all within your paid 8 hour day.
Is an acute care residency worth it?
Residency is a very large topic in universities currently and their are many mixed emotions about it. Of the therapists surveyed 66% were specialized in at least one area of interest (orthopedics, cardiovascular and pulmonary, and geriatrics). But 0% did a residency program.
Acute care physical therapists have the option to participate in several residency programs and specialize in a specific treatment area. There are “acute care residency” programs even one offered by Johns Hopkins University. You can even attend one in other areas such as neurology, orthopedics, and cardiovascular and pulmonary and become a specialist in a hospital if that role is available.
A common reason for not completing residency programs were finances. The collective feeling was why spend money or lose out on earning potential when I can work and get the same experience. A downside to this thought is it takes slightly longer to specialize.
One therapist says “I rather get my experience in a certain specialty working and get paid”
This is a very common thought across older and new therapist. As you already know or soon will know, it is very expensive and long process to get a DPT. Why lose money when you are not expected to earn any more money with or without a specialization/residency. Talking to clinic owners I can tell you, many do not care about your residency. The ones that do will not pay you more unless you bring real value to the clinic not just a 12 month extension of school.
Frequently asked questions

How does an acute care physical therapist contribute to discharge planning?
After a physical therapist evaluates a patient they make a discharge recommendation based on the current ability of the patient and how the might progress during their time in the hospital. Since physical therapists are experts in movement and mobility there opinions hold a high influence, but the final medical decision is made by the medical doctor.
What are physical therapy outcome measures used in acute care?
Outcome measure that are commonly used in the acute setting are the tinetti, Berg Balance Scale, four square step test, 10m walk test, 2 minute walk test, 5 times chair rise, and 30 second sit to stand.
Why work in acute care physical therapy instead of other settings (inpatient rehab, outpatient) etc?
Someone might chose to work in acute care physical therapy because they want a fast pace, flexible schedule, and see a variety of patients. They may also want the benefits associated with working for a hospital.
Someone may chose another setting based on the reasons explained earlier in this post, but generally to see a higher level patient, see long term progress, or work in private practice.
Do acute care PTs get a chance to really spend time and foster relationships with their patients?
Yes you will spend time and foster relationships with your patients. This can be limited due to the acute nature of the hospital. That may be a good thing because if you have more time to create a relationship this means the patient is not progressing enough to go home. You will not get to spend as much time with the patients as you would in outpatient, but that is not always a bad thing.
What are some exercises/activities an acute care PT administer with a patient?
The main activity you will perform with a patient in the acute setting is bed mobility (rolling, supine to sit, scooting, and sitting edge of bed), transfers (sit to stand, stand pivots, squat pivots, etc), gait training, and stair negotiation. After that if there is time remaining you may do therapeutic exercise such as ankle pumps, quad sets, squat, etc.
What are some challenges and brain stimulating parts of being an acute care PT?
There are a couple major challenges in this setting.
- Determining if it is safe to treat or progress a patient. You will need to know physiology extensively and determine how your patient may respond to your intervention.
- Deciding the most appropriate discharge recommendation. The challenge is balancing safety, financial obligations, and patient autonomy.
- Dealing with the emotions of an acute injury. Imagine being 25 with your whole life ahead of you, then have a forever life changing event such as becoming a quadriplegic. You are one of the first people to interact with that person as they realize their life has changed forever.
Do you have to deal with bodily fluids and poop at times?
Yes. Simple as that. It will be a at minimum weekly occurrence, but it is just part of the job.
Are acute care therapist’s ever on call?
No
How many evaluations does an acute care physical therapist see a day?
This is dependent on the day and need of the hospital. Could be up to 6 on a bad day. These are not terrible as documentation is similar for follow ups and evaluations.
References
(1) Castro-Avila AC, Serón P, Fan E, Gaete M, Mickan S. Effect of early rehabilitation during intensive care unit stay on functional status: systematic review and meta-analysis. PloS one. 2015;10(7):e0130722. Doi: 10.1371/journal.pone.0130722

